What is “Syncope”?
“Syncope” means loss of consciousness due to decreased blood supply to the brain. “Syncope” is the most important and common Seizure Mimic.
Some events look almost precisely like seizures but are not seizures. These events are called “Seizure Mimics”, and may be mistaken for seizures.
There is NO electrical surge in the brain with any of these “Seizure Mimics”.
If an episode of Syncope is mistaken for a Seizure, two things happen: Unnecessary treatment with anti-epileptics, and lack of treatment for the “true” condition (e.g. cardiac arrhythmia).
Which problems cause “Syncope”?
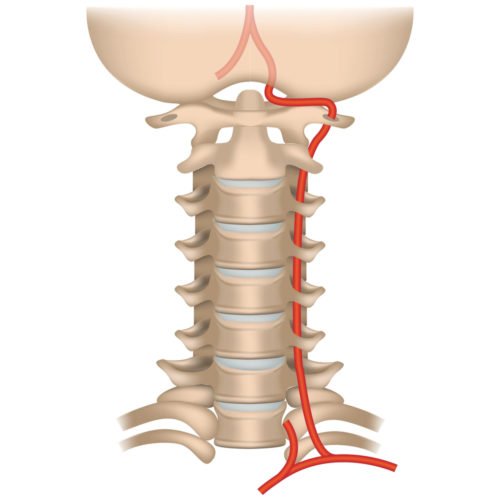
Lets quickly summarize how blood goes to the brain: The heart receives oxygenated blood from the lungs. It pumps this blood to the brain through large blood vessels in the neck.
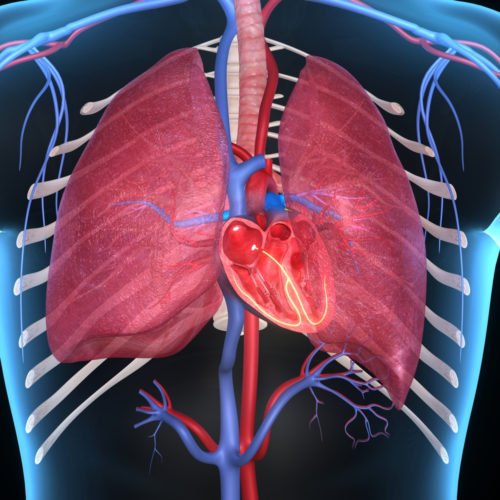
4 Groups of problems can cause Syncope:
– Overactivity of the vagal nerve
– A sudden drop in BP on standing up (Orthostatic Hypotension)
– Problems with blood vessels going to the brain
Which heart problems can cause Syncope?
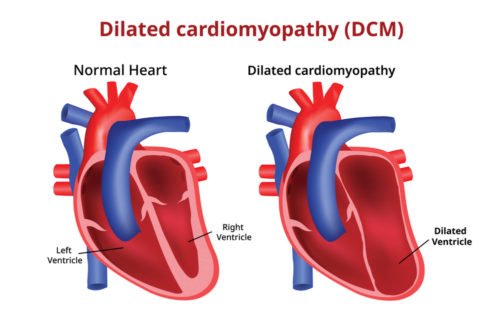
- If the heart has become weak (for example due to multiple heart attacks) and not able to pump enough blood, the patient may occasionally lose consciousness. This cause is not very common.

A weak heart can cause episodes of unconciousness (syncope) - More common is an obstruction to blood flow in the heart.
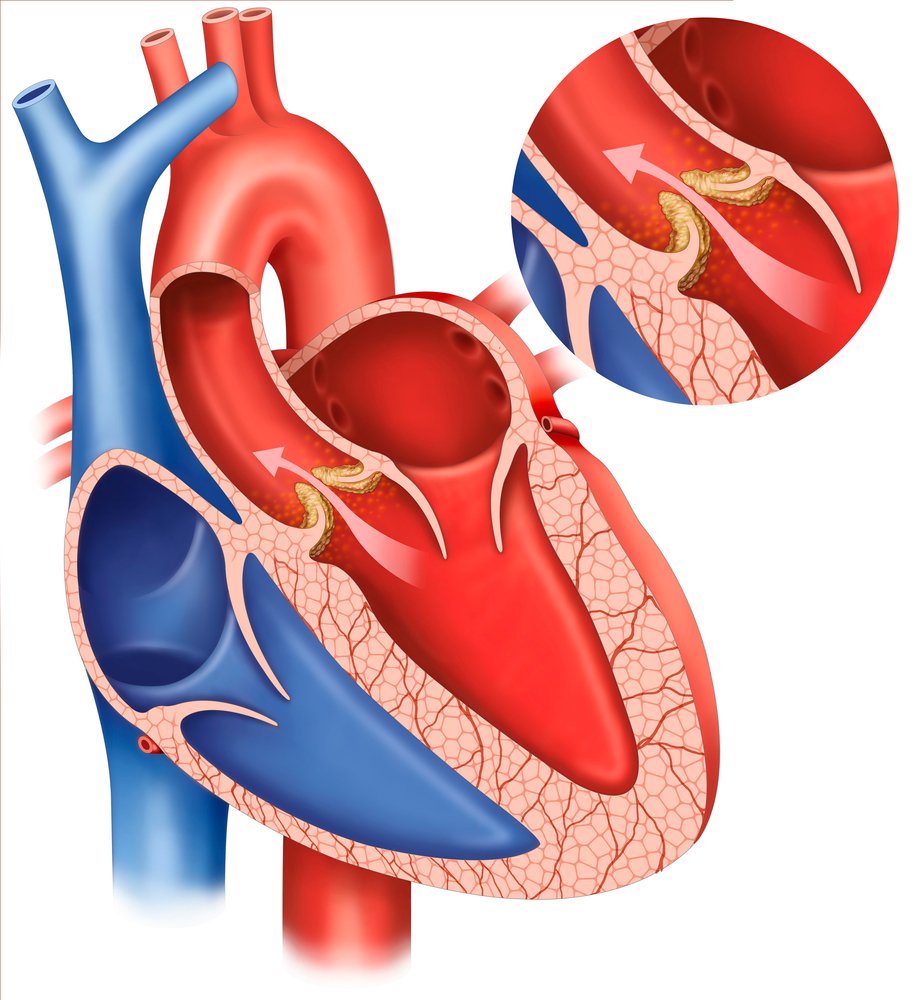
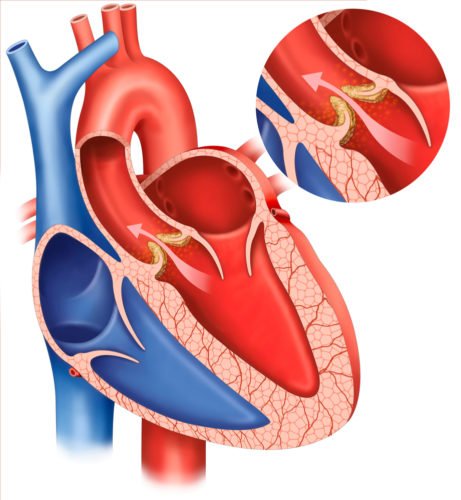
Valves in the heart usually keep blood moving in only one direction. They can open and close as needed. Sometimes the heart valves (especially a valve called the Aortic Valve) may become damaged and incapable of opening completely – this decreases blood flow to the brain. Sometimes, the heart wall around the Aortic Valve may become thickened producing the same effect – this condition is called “Hypertrophic Sub-Aortic Stenosis”.
An echocardiogram quickly & easily detects these structural problems.
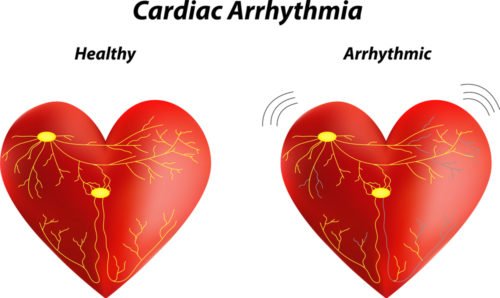
Valve problems in the heart may obstruct the flow of blood and cause episodes of unconciousness (syncope) - A straightforward problem to miss is Cardiac Arrhythmia. Usually, the heart beats regularly, almost like a clock. But if the wiring system of the heart develops problems, it may have episodes where it suddenly stops beating or starts beating very rapidly without pumping any blood. This condition is called a cardiac Arrhythmia (A = lack of – rhythm).
Since these rhythm problems occur only once in a while, a single ECG may miss them. Therefore, an EEG machine that is stuck to your chest and records your heart rhythm for many days (A Holter Monitor) may be required. Newer devices called External Loop Recorders (ELDs) can record your heart rhythms for many months at one time!
You may require a pacemaker if you have a severe cardiac arrhythmia.
An irregularly beating heart can cause unconciousness (syncope)
What do you mean by overactivity of the Vagal Nerve?
The vagal nerve is a long nerve from the brain to the heart. When it is active, it can decrease the heart rate.
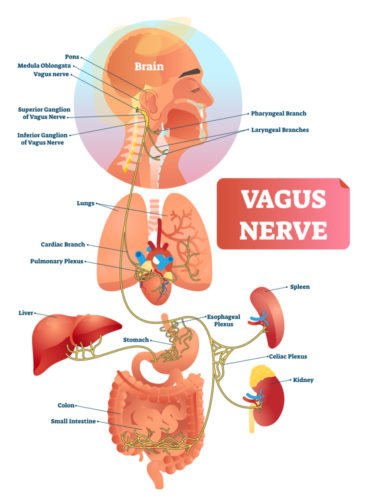
If something overstimulates the vagal nerve, it can become overactive. It then causes the heart to become very, very slow. This causes decreased blood flow to the brain and leads to loss of consciousness.
It is easy to identify the precipitant that caused the vagus nerve overactivity. The following is a list of such precipitants. Only the first one is common:
- Intense Emotion or Pain: Being startled, the sight of blood, intense fear etc
- Choking on something. Rarely swallowing very cold or hot food can cause Syncope.
- Massaging the neck or wearing a very tight collar (which leads to stimulation of sensors called carotid bodies which are connected to the vagus nerve)
- Passing urine (Micturition Syncope)
- Rarely: Laughing hard and Orgasms
What can cause a sudden drop in Blood Pressure on standing (Orthostatic Hypotension)?
Hypo = Low, Tension = Pressure
Meaning: Low Pressure on Standing Straight
When we stand up suddenly, blood tends to pool in our legs, and our brain tends to get less blood. To prevent this, the blood vessels in our legs contract and our heart beats faster. If these things don’t happen, our heart pumps less blood, and our blood pressure drops. This may cause us to lose consciousness.
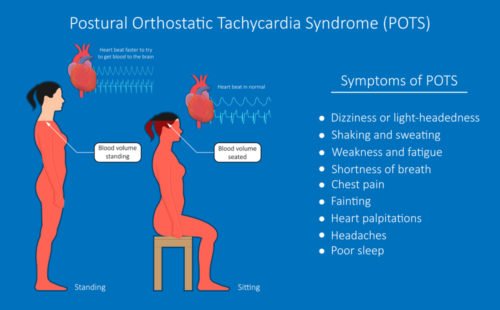
A sudden and large drop in our Blood Pressure on getting up suddenly is called “Orthostatic Hypotension”.
During your office visit, the doctor may check your BP when you are lying down and then ask you to get up suddenly. While you are standing, he/she will check your BP two more times. If your upper (systolic) BP drops by more than 20 units, or your lower (diastolic) BP drops by more than 10 units, its likely that your events are due to Orthostatic Hypotension.
In some cases, an advanced test called a “Tilt Table Test” confirm the diagnosis.
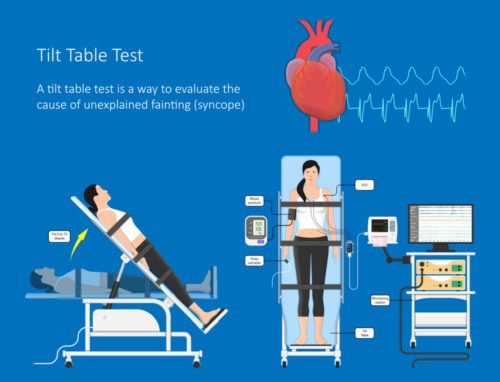
What can cause this drop in BP? There are many causes! It is difficult to remember all of these causes, but I list them here so that you can understand the monumental task facing your doctor and are patient while he goes through a series of tests to find the exact cause of your orthostatic hypotension:
Causes of Orthostatic Hypotension | Examples |
| Brain Problems | – Parkinson’s disease and its sisters like MSA – As part of normal ageing |
| Nerve problems (Neuropathy) | Damage to nerves controlling the heart & blood vessels due to: – Alcoholism – Diabetes – B12 deficiency – HIV – Many others… |
| Heart Problems | – Cardiac failure – Valve problems |
| Dehydration
| Not enough fluid in the body due to: – Drinking very little water – Diarrhoea or vomiting |
| Hormonal Problems | – Low functioning of the Adrenals (Addison’s) – Low thyroid levels – Pheochromocytoma |
| Medications | Many, many medications including: – Blood pressure medications – Antidepressants – Anti-parkinson’s medications Click here for a: [longer list] |
The best treatment of Orthostatic Syncope is the treatment of the underlying problem, e.g. replacing the problematic medication. In some cases, medications such a Fludrocortisone, Midodrine or Pyridostigmine may be useful.
What problems with blood vessels can cause Syncope?
Usually problems with blood vessels going to the brain present with a stroke, with weakness on one side of the body. Blood vessel problems presenting only with episodes of unconsciousness and being confused with seizures are rare. Therefore, these are only briefly described below:
- If the blood vessels going to the brain – especially the carotid arteries described above – become narrow (e.g. due to accumulation of cholesterol) then the person may have episodes of sudden unconsciousness.

Rarely, if an artery going to the brain is narrow or is misconnected to the arm vessels, you may have repeated episodes of unconciousness (syncope). - Occasionally when blood that is going to head is shunted away to the arm, the person may get episodes of unconsciousness whenever he/she uses that arm. This condition is called Subclavian Steal syndrome.
| Caution: This information is not a substitute for professional care. Do not change your medications/treatment without your doctor's permission. |
 Dr. Siddharth KharkarDr. Siddharth Kharkar has been recognized as one of the best neurologists in Mumbai by Outlook India magazine and India today Magazine. He is a board certified (American Board of Psychiatry & Neurology certified) Neurologist. Dr. Siddharth Kharkar is a Epilepsy specialist in Mumbai & Parkinson's specialist in Mumbai, Maharashtra, India. He has trained in the best institutions in India, US and UK including KEM hospital in Mumbai, Johns Hopkins University in Baltimore, University of California at San Francisco (UCSF), USA & Kings College in London. |
 Skip to content
Skip to content